Boost Patient Survey Scores with Patient Engagement Tools
Patients who feel informed and heard rate their care experience significantly higher — and the data backs this up. According to HCAHPS results consistently reported by the Centers for Medicare & Medicaid Services (CMS), communication with nurses and doctors ranks among the lowest-scoring domains across U.S. hospitals. That’s not just a patient experience problem. For hospital administrators and clinical managers, low patient satisfaction survey scores directly affect reimbursement rates, accreditation standing, and institutional reputation.
The link between healthcare communication and patient outcomes is well-documented. When patients don’t understand their care plan, feel ignored by staff, or receive conflicting information, scores fall — and so does trust. Focusing on patient-centered communication strategies is essential to improve satisfaction and outcomes. Yet many facilities continue to address these gaps reactively, rather than building the systems and tools that prevent them.
This post covers what you need to know about patient surveys, which domains matter most, and how patient-centered care tools — from bedside communication boards to structured nursing communication strategies — can produce measurable, sustained improvements in scores. Healthcare providers are encouraged to add new digital patient engagement tools to their existing systems to enhance patient involvement. Digital tools drive the best results through cost-effective automation.
What Are Patient Satisfaction Surveys — and Why Do They Matter?
Patient surveys are structured tools used to measure how patients perceive the quality of their care experience. They capture feedback across key domains: communication, responsiveness, environment, discharge planning, and overall care quality. Hospitals use this data to identify service gaps, benchmark performance, and guide quality improvement initiatives.
The most commonly used survey types include:
- HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems): The federal gold standard for inpatient satisfaction measurement. HCAHPS results are publicly reported and directly tied to CMS Value-Based Purchasing (VBP) reimbursements — making them a financial priority for any facility participating in Medicare and Medicaid programs.
- Press Ganey Surveys: Widely adopted by hospitals to benchmark patient experience performance against peer institutions, with detailed analytics to support targeted improvement.
- CG-CAHPS: Focuses on outpatient and physician office settings, measuring communication quality in ambulatory care environments.
- Post-discharge surveys: Short, targeted questionnaires sent after a patient leaves the facility to capture real-time feedback on the care transition experience.
Under the CMS VBP Program, a portion of a hospital’s Medicare reimbursement is withheld and redistributed based on performance — including patient experience scores. Facilities that score below their peers face direct financial consequences. This makes improving survey results not only a clinical priority, but an operational and revenue-related one.
Consistently, the domains with the lowest scores across survey types center on communication with nurses and physicians. That makes healthcare communication the highest-leverage area for improvement — and the logical starting point for any patient perception strategy.
Common Patient Satisfaction Survey Question Examples (and What They’re Really Measuring)
Understanding the specific questions that appear on these surveys helps clinical teams connect daily behaviors to measurable outcomes. Here are representative questions from the communication domain:
| Survey Domain | Example Question | What It Measures |
|---|---|---|
| Communication with Nurses | “How often did nurses explain things in a way you could understand?” | Clarity and accessibility of nurse-patient communication |
| Communication with Nurses | “How often did nurses listen carefully to you?” | Patient perception of attentiveness and empathy |
| Care Information | “How often were you informed about what to expect during your stay?” | Transparency and proactive communication |
| Medication Communication | “Did hospital staff tell you what the medicine was for?” | Care coordination and patient education |
| Care Transitions | “Did staff explain the purpose of medicines you would take at home?” | Discharge readiness and follow-through |
What these questions collectively reveal is that patients don’t just evaluate whether care was clinically competent — they evaluate whether they felt like active participants in it. Tailoring care to the individual is essential for fostering engagement and optimizing outcomes. Patient-reported outcome tools like InteliChart collect clinical data directly from patients, enabling healthcare teams to personalize communication and care coordination based on each individual’s needs and preferences. Communication gaps, inconsistent information, and a perceived lack of attentiveness are the most common drivers of low scores.
For hospital administrators procuring patient-centered care tools, these questions form the benchmark. Any solution worth implementing should directly support higher performance across these domains.
How Patient-Centered Care Tools Improve Survey Scores
Patient-centered care tools are solutions designed to keep patients informed, engaged, and involved in their own care. These tools provide patients with essential information and support, helping them better understand their treatment and care process. Patient education aims to give consumers the foundational knowledge they need about their health and healthcare options. When implemented consistently, they create a proactive, transparent care environment — one where patients know who is caring for them, what the plan is, and what to expect next.
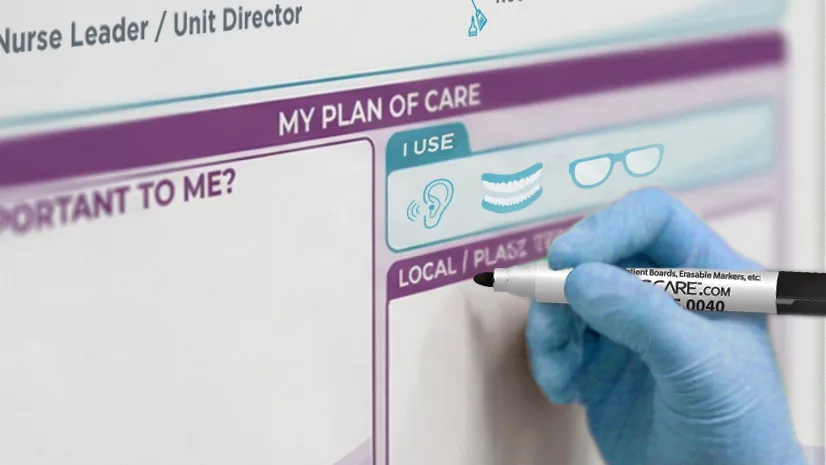
Bedside Communication Boards
Bedside communication boards — also called patient communication boards or whiteboard systems — are among the most widely adopted and evidence-supported patient engagement tools for improving HCAHPS scores. Positioned at the bedside or in the patient’s direct line of sight, these boards display real-time, personalized information including:
- Care team names and roles
- Daily care goals
- Current medications and pain levels
- Discharge plans and anticipated timelines
Patient communication boards can be customized with various sizes, colors, and graphics to meet the needs of each department or branding requirements. CareBoards patient communication boards feature interchangeable, magnet receptive dry-erase surfaces. These boards are created and developed to enhance communication, safety, and responsiveness in healthcare settings. A set of communication boards can be used throughout a facility to ensure consistency and clarity. Many customers have reported positive experiences with our company, noting the high product quality and support provided during the purchasing and installation process. Healthcare communication boards help engage patients and their families in the care process and provide a clear understanding of care plans.
The direct connection to HCAHPS domains like “communication with nurses” and “care transitions” is clear: when patients can see their care plan, updated throughout the day, they feel informed — and they report it. For a detailed look at how these tools transform care interactions, explore 7 Ways Bedside Communication Transforms Patient Experience.
Visual Communication in Healthcare
Not all patients process written information the same way. For patients with low health literacy, language barriers, or cognitive challenges, simple visual communication tools — including iconography, color-coded information, and multilingual content — significantly reduce confusion, enhance patient understanding, and reduce errors.
Visual aids also support compliance with patient rights standards and CMS requirements for informed consent and care education, reducing institutional risk alongside improving patient experience. Language translation technology ensures every patient receives the same level of care and engagement, regardless of language.
Digital Patient Engagement Tools
Technology-enabled solutions, including patient portals, interactive bedside TVs, and nurse call integrations, extend the reach of patient communication beyond the bedside. Email is used as a secure, HIPAA-compliant channel for personalized outreach, notifications, and two-way communication, enhancing patient engagement. When patients can access their care plan, review test results, or flag concerns through a dedicated interface, their sense of agency increases. Mobile health apps facilitate 24/7 access to care teams for quick inquiries, while telehealth platforms provide virtual, face-to-face communication essential for accessibility. Digital tools also enable patients to schedule appointments and follow up with their doctor virtually. Secure patient portals allow patients to view medical records, lab results, and securely message providers, serving as centralized hubs for accessing medical records and care plans 24/7. Remote patient monitoring tools allow healthcare providers to monitor patient health data in real-time using wearable devices. Telehealth and virtual care platforms enable effective remote consultations and chronic disease management. AI-powered chatbots offer instant support to patients for routine interactions, and AI-powered virtual assistants can handle routine inquiries and schedule appointments 24/7. Research consistently links higher patient engagement to reduced anxiety, better adherence to care plans, and improved scores.
For more information about digital patient engagement tools, click here.
Nurse-Patient Communication Strategies That Drive Better Outcomes
Tools create the infrastructure for good communication — but communication itself is both a skill and a system. Facilities that see sustained score improvements treat it as both.
Evidence-based nurse-patient communication strategies that consistently perform well include:
- Hourly Rounding: Proactive check-ins at regular intervals reduce call light usage and improve patients’ perception of staff attentiveness — directly affecting HCAHPS responses about nurse communication.
- AIDET Framework: A structured communication model — Acknowledge, Introduce, Duration, Explanation, Thank You — that standardizes patient interactions and reduces variability between staff members.
- Teach-Back Method: After providing discharge instructions or medication education, nurses ask patients to repeat the information in their own words. This confirms comprehension and supports higher scores on care transition questions.
- Collaborative Whiteboard Goal-Setting: Involving patients in setting daily care goals on the communication board shifts the dynamic from passive recipient to active participant — a shift patients notice and report in surveys. Encouraging healthcare providers, staff, patients, and families to collaborate on these goals enhances care coordination, improves patient satisfaction, and fosters a supportive environment.
Follow-up contacts provide the chance to strengthen and reestablish patient engagement after a healthcare visit.
A critical factor in any of these strategies is adoption. Tools and frameworks that require extensive training or complex workflows see inconsistent use, especially across high-turnover environments. Prioritizing user-friendly, minimal-training solutions increases the likelihood that staff apply them consistently across shifts.
Care Coordination and Management: Bridging Gaps for Higher Satisfaction
We understand that delivering exceptional patient care in today’s hospitals feels like navigating a complex maze—and we know how challenging it can be when your patients interact with so many different caregivers, physicians, and support staff during their stay. Without a clear way to share information, those crucial details about treatment plans have a way of slipping through the cracks, leaving everyone feeling a bit lost and frustrated. We’ve seen how this can impact the patient experience you work so hard to create.
Here’s where patient communication boards step in as your trusted ally. Think of them as that reliable friend who always keeps everyone in the loop—they provide a centralized, visible hub right in each patient room where everyone involved in care can stay connected. We’re talking about family members, nurses, doctors—the whole team having instant access to daily care goals, scheduled events, medication updates, and key contact information. When your patients and their families can easily see and understand what’s happening next, something wonderful occurs: they feel genuinely in control and confident about their care journey.
We love hearing from hospitals that have made this shift because the results speak for themselves—not only do patients communicate better, but staff collaboration becomes so much smoother. Picture this: your caregivers can quickly glance at the board to confirm what’s been discussed, see what needs to happen next, and know exactly who’s handling each step. This simple approach helps you avoid those frustrating miscommunications, missed tasks, and unnecessary repetitions that can really impact how patients feel about their experience with you.
By making the care process transparent and accessible, these communication boards transform your patients and families from passive recipients into active participants in their health journey. We know this sense of involvement and clarity is exactly what drives those higher patient scores you’re working toward. When you invest in effective communication tools like these boards, you’re really empowering your hospital to deliver the kind of care that makes a difference—better outcomes, happier patients, and the satisfaction scores that reflect the quality care you’re already providing.
Choosing the Right Patient Satisfaction Solutions for Your Facility
No two facilities have the same patient population, staffing model, or budget — and the solutions that work best reflect those differences. When evaluating patient satisfaction solutions, consider the following:
| Consideration | Key Questions |
|---|---|
| Customizability | Can the solution be tailored to different department workflows and patient demographics? |
| Integration | Does it connect seamlessly with your existing EHR/EMR systems? |
| Compliance | Does it meet HIPAA requirements and relevant CMS standards? |
| ROI | What measurable improvements have similar facilities reported in survey scores or operational efficiency? Customers frequently report positive feedback and increased satisfaction from patients, families, and staff when using patient engagement tools. |
| Ease of Use | Does it require minimal staff training to ensure consistent, high-adoption implementation? |
| Scalability | Can it grow with your facility or expand across multiple units? |
It’s important to remember that what may seem impossible in healthcare coverage or patient engagement can often be achieved with the right tools and education. Tracking the number of overdue payments, collections, or copay notifications can help improve financial management and operational efficiency. Ensuring that patient instructions and processes are followed as intended supports better compliance and outcomes. Automated prescription notifications also help patients know when their prescriptions are ready for pick-up and how to take their medication.
Before committing to a facility-wide rollout, pilot the solution in a single unit. This allows your team to collect early performance data, identify workflow friction points, and build an internal case for broader adoption — reducing change resistance and improving long-term outcomes.

Turn Survey Scores into a Catalyst for Better Care
Patient surveys measure what patients actually experience: whether they felt heard, informed, and respected during their care. The most common low-scoring domains — communication with nurses, medication education, and care transitions — are also the most actionable.
The right patient-centered care tools, from bedside communication boards to structured nurse-patient communication frameworks, directly address these gaps. They create environments where patients are active participants in their care, not passive recipients. Follow-up contacts are especially important for people who may feel stressed or concerned after a healthcare visit, helping to support their understanding and engagement. Organizations that invest in patient-centered care tools consistently see improved outcomes and higher satisfaction among patients and staff. Facilities report great results and experiences using these patient engagement tools, noting better communication and overall care quality. Health technologies empower patients, leading to lower overall healthcare costs. And when staff have reliable, user-friendly systems to support consistent communication, scores improve — not as a one-time spike, but as a sustained trend.
The business case is equally compelling. Better HCAHPS and Press Ganey scores support stronger reimbursement performance under value-based purchasing models, improve accreditation positioning, and enable competitive benchmarking against peer institutions.
Start by auditing your current communication tools and identifying one domain — whether that’s nurse communication, medication education, or discharge planning — where a structured improvement could move the needle. Small, targeted changes often produce the most immediate and measurable results.
Ready to improve your facility’s patient survey scores? Explore VisiCare’s patient-centered care solutions and book a consultation to find out how the right tools can make a measurable difference for your patients, your staff, and your bottom line.
Frequently Asked Questions
How do communication boards improve HCAHPS scores?Bedside communication boards directly support higher scores in HCAHPS domains like “communication with nurses” and “care transitions” by displaying real-time, personalized patient information — including care team names, daily goals, medications, and discharge plans. When patients can clearly see and reference this information, they report feeling more informed and engaged, which is precisely what survey questions in these domains are measuring.
What tools improve patient satisfaction scores in hospitals?The most impactful tools include bedside communication boards, visual communication aids, structured nursing communication frameworks (like AIDET and hourly rounding), and digital engagement tools such as patient portals and interactive TVs. Patient engagement tools can cover multiple aspects of a patient’s well-being, including physical, emotional, and lifestyle factors, providing a comprehensive approach to care. The common thread: they all reduce communication gaps between clinical staff and patients.
Why do communication domains score the lowest on patient satisfaction surveys?Communication gaps are common in high-pressure clinical environments, where staff manage multiple patients and documentation demands simultaneously. Without structured tools and systems to standardize patient interactions, communication becomes inconsistent across shifts — and patients notice. Survey scores in communication domains reflect this variability more clearly than almost any other area.
How long does it take to see improvement in patient survey scores after implementing new tools?Results vary by facility, but hospitals that implement structured communication tools alongside consistent staff training typically begin to see measurable score improvements within one to two survey cycles. Piloting solutions in a single unit before a full rollout helps establish a baseline and build early evidence of impact.


