More Than Words for Clearer Communication in Mental Health
In mental health care, communication is not just part of the treatment—it is the treatment. How clinicians and staff communicate with patients can either build a therapeutic alliance or break it. Patients experiencing a mental health crisis often grapple with anxiety, distrust, and difficulty with verbal processing. These challenges can make traditional communication methods less effective and sometimes even counterproductive.
To foster genuine healing and safety, facilities must adopt a more holistic framework that promotes patient empowerment. This article explores a multi-layered approach to mental health communication that goes beyond words. By integrating empathetic verbal techniques, clear visual aids like custom patient boards, and supportive environmental design, healthcare facilities can create a truly therapeutic space for recovery where patients can actively participate in their care.
Communication in Behavioral Health and Emergency Department Settings
Effective communication is especially critical in hospital behavioral health units and emergency departments, where high-stress situations demand precision, empathy, and safety. These environments often cater to individuals in acute mental health crises, requiring a tailored approach to ensure patient and staff well-being. Miscommunication or ineffective interactions can exacerbate a patient’s distress, increasing the potential outcomes of conflict or inhibiting their ability to engage with care plans.
Emergency departments face unique challenges, with high patient turnover and a broad range of conditions being treated simultaneously. The fast-paced nature of these settings can result in heightened anxiety for patients, particularly those navigating a mental health crisis. Behavioral health units, while more specialized, require consistent and clear communication strategies to build trust and provide a sense of security. Incorporating tools and processes designed to address these needs, such as those outlined in resources like partners in communication design for AEC, can help design safer environments that prioritize communication as a key factor of care. By doing so, hospitals can foster more effective therapeutic interactions and better patient outcomes.
Building Trust Through Words: The Art of Therapeutic Conversation
The foundation of any therapeutic relationship is trust, and that trust is built through careful and empathetic verbal communication. For patients who feel vulnerable or unheard, the right words can de-escalate anxiety and validate their experience, providing essential emotional support.
Active Listening and Validation
Active listening is more than just hearing words; it is about understanding the meaning and emotion behind them. It involves techniques like paraphrasing what the patient has said (“So, what I’m hearing you say is…”) to confirm understanding and reflecting their feelings (“That sounds incredibly difficult.”). These validating statements show the patient that their perspective is seen and respected, which is a crucial step in building rapport and enhancing patient empowerment.
Trauma-Informed Language
A trauma-informed approach shifts the focus from “What’s wrong with you?” to “What happened to you?” This simple change in language reframes the conversation from one of judgment to one of compassion. It involves using person-first language (e.g., “a person with schizophrenia” instead of “a schizophrenic”) and avoiding labels that can feel stigmatizing. Emphasizing choice and collaboration in every interaction reinforces that the patient is a partner in their own care.
Simple, Clear, and Consistent Messaging
During a crisis, a person’s ability to process complex information is often diminished. Clinicians should use short, simple sentences and avoid clinical jargon. Just as important is consistency. When every member of the care team provides the same information about schedules, medications, and treatment plans, it reduces confusion and builds a sense of security for the patient.
Strategies for Family Members in Patient Engagement
Family members play a crucial role in supporting patients throughout their healthcare journey. Research shows that when patients and their families actively engage with healthcare teams, outcomes improve, satisfaction increases, and healthcare costs can be reduced. The Institute of Medicine (IOM) emphasizes that involving patients, families, and caregivers as full participants in care leads to better health experiences and economic results. However, despite these benefits, patient and family participation in care decisions remains limited.
Effective family engagement strategies include fostering partnerships between families and healthcare providers, recognizing families as essential members of the care team, and valuing their insights and perspectives in care planning and decision-making. The National Partnership for Women & Families highlights collaborative patient and family engagement at multiple levels: direct care, organizational quality improvement, community involvement, and policy development.
Family-centered care underscores the importance of respecting patients’ definitions of family and involving them according to patient preferences. This approach enhances communication, supports shared decision-making, and promotes patient empowerment.
Safety is another key benefit of family engagement. The National Patient Safety Foundation’s Lucian Leape Institute reports that partnerships between care providers and families contribute significantly to safer care environments. Overcoming barriers to family involvement requires leadership commitment and systems that encourage open communication and collaboration.
In practice, healthcare facilities can support family engagement by providing clear information, encouraging family participation in care discussions, and creating welcoming environments that respect diverse family structures. These efforts align with the Triple Aim framework, which seeks to improve care experience, population health, and reduce costs through patient- and family-centered care.
For more detailed guidance on family engagement strategies and definitions, see the comprehensive report by the Institute for Patient- and Family-Centered Care. Patient and Family Engagement Strategies and Definitions
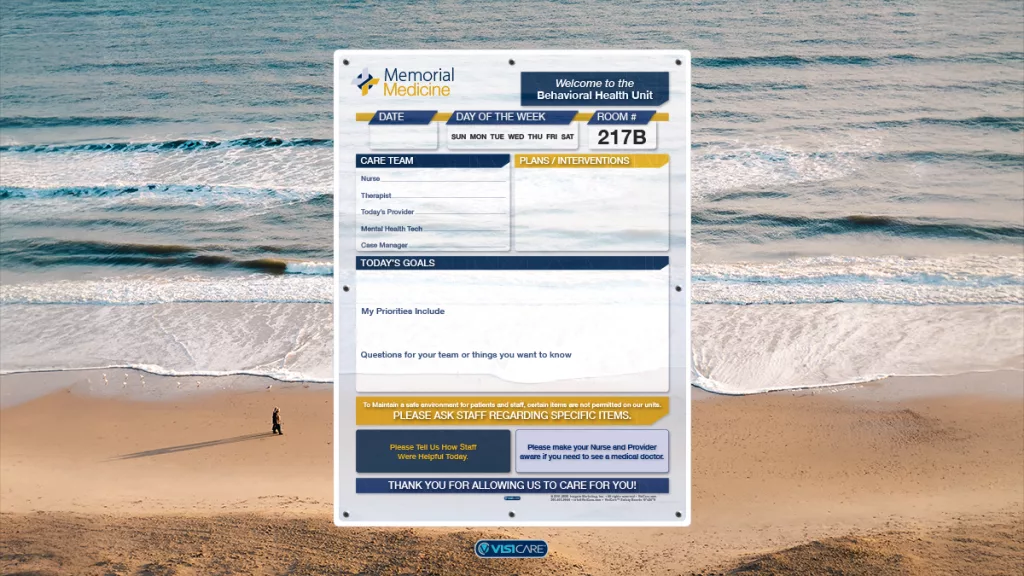
Making Care Visible: How Custom Patient Boards Empower Patients
Verbal communication can be fleeting, but visual anchors provide a constant, reliable source of information that patients can turn to at any time. Custom patient boards are not just informational tools; they are essential visual aids that ground patients in their care plan and reduce the profound anxiety that comes from uncertainty, reinforcing patient empowerment.
Reducing Anxiety by Answering Unasked Questions
For a patient in a mental health facility, the “unknown” can be a significant source of distress. A well-designed patient board answers their unasked questions at a glance: Who is my nurse today? What time is group therapy? What is the goal for today? This predictability creates a sense of safety and routine, which is foundational to a therapeutic environment.
Facilitating Shared Decision-Making
Patient boards can be transformed from static displays into interactive tools for mental health communication. By including sections for “My Goals” or “Questions for My Doctor,” the board gives patients a tangible way to voice their needs and actively participate in their treatment. This simple feature helps shift the dynamic, turning patients from passive recipients of care into active partners in their recovery journey.
Discreetly Communicating Safety Cues
In a mental health setting, clear communication among staff is critical for safety. Patient boards can facilitate this with standardized, discreet visual cues. For example, a small, color-coded magnet could signify a fall risk, a specific dietary need, or a non-verbal status. This system allows staff to quickly get vital information without using stigmatizing language or compromising the patient’s dignity. Is your facility’s patient board an active tool for therapeutic communication or just a static display?
Designing for Calm: How the Environment Speaks to Patients
The physical environment is a silent communicator. Through non-verbal sensory cues, a facility’s design tells patients whether they are in a place of safety and respect or one of confinement and stress. The environment also supports physical health by reducing stress and promoting healing.
The Impact of Color, Light, and Sound
Sensory inputs have a direct impact on a person’s psychological state. Research in evidence-based design shows that soft, cool color palettes like blues and greens can have a calming effect. Conversely, harsh fluorescent lighting and loud, echoing acoustics can be agitating. Facilities should prioritize maximizing natural light, using adjustable and glare-free lighting, and incorporating sound-dampening materials like acoustic ceiling tiles and wall panels.
Biophilia: The Healing Connection to Nature
Biophilic design involves incorporating elements of nature into the built environment. This connection to nature has been shown to reduce stress and improve mood. Even when direct access to the outdoors is not possible, this can be achieved through secured, large-scale nature-themed artwork, the safe inclusion of plant life, and the use of natural materials like wood-look flooring and finishes.
Providing Choice and Control in Personal Space
An environment can communicate trust and respect by giving patients a sense of control. This does not have to be complicated. It can be as simple as providing tamper-proof lighting dimmers in patient rooms, offering movable (but safe and weighted) seating in common areas, or creating designated quiet zones away from high-traffic corridors. These small measures of autonomy can be incredibly empowering for a patient who may feel they have little control over their situation.

A New Ecosystem of Care for Mental Health Communication
Effective solutions in a three-pronged approach. It is spoken through empathetic verbal skills, seen through clear visual aids like patient boards, and felt through a supportive and calming environmental design. When these three layers are not aligned, patients receive mixed signals that can erode trust and hinder progress.
We encourage facility leaders to perform a “communication audit.” Ask yourselves: Do our verbal practices build trust? Do our visual tools empower patients? Does our environment promote calm? By aligning these communication strategies, healthcare facilities can create a cohesive ecosystem of care that enhances patient safety, fosters genuine connection, and accelerates the path to recovery.
This approach aligns the importance of integrated communication and environmental design in improving mental health outcomes. Such strategies not only enhance emotional well-being but also encourage patients to actively participate in their care, improving overall treatment effectiveness including in contexts like clinical trials.
By prioritizing communication as a key factor in mental health care, facilities can provide the emotional support and empowerment patients need to navigate their journey toward better physical health and recovery.


