The Role of Visual Communication in Reducing Medical Errors
Despite advancements in technology and medicine, medical errors remain a startlingly common occurrence. According to studies by Johns Hopkins, medical errors are the third leading cause of death in the United States, claiming over 250,000 lives annually. While this statistic is sobering, the root cause is often not a lack of medical knowledge, but a breakdown in communication. The consequences of medical errors can result in significant patient harm, including physical injury, prolonged recovery, and even loss of life.
Complex medical data, rushed handoffs, and high-stress environments create a perfect storm for misunderstandings. The global burden of medical errors extends beyond individual hospitals, impacting health systems worldwide and contributing to increased morbidity, mortality, and economic costs.
Approximately 400,000 hospitalized patients experience some preventable harm each year in the US, highlighting the urgent need for targeted safety protocols for hospitalized patients.
Visual communication plays a pivotal role in reducing medical errors by ensuring critical information is clearly conveyed and easily accessible to both patients and healthcare providers. The financial burden of medication errors alone is approximately $42 billion annually, with hospital-acquired infections costing up to $45 billion per year. Studies published in reputable sources such as Jama Health Forum and National Academies Press emphasize that reducing medical errors not only improves patient safety but also alleviates the financial burden on patients, families, and health systems.
Tools like patient communication boards and visual aids do more than just decorate a room; they enhance clarity, minimize misunderstandings, and improve overall safety in high-stakes medical environments. Patients affected by medical errors might experience severe psychological distress, including PTSD, depression, and a loss of trust in the healthcare system.
Understanding Medical Errors
To solve the problem, we must first understand it. A medical error is a preventable adverse effect of care, whether or not it is evident or harmful to the patient. These can range from minor mix-ups to catastrophic events.
Common types of medical errors include:
- Medication Errors: Administering the wrong drug, dosage, or route, or giving potentially dangerous combinations of medications. Medication errors affect 1 out of every 30 patients in healthcare, with more than a quarter of this harm regarded as severe or life-threatening.
- Surgical Errors: Classified as ‘never events’, these include wrong-site surgeries and leaving surgical instruments inside a patient. Surgical errors account for 10% of preventable patient harm in healthcare settings.
- Diagnostic Errors: Missed, wrong, or delayed diagnoses. Diagnostic errors occur in 5–20% of physician-patient encounters, with harmful diagnostic errors found in a minimum of 0.7% of adult admissions. (Diagnostic errors are a complex issue, and the exact prevalence depends on the definition and measurement methods used.)
- Equipment Failures: Malfunctioning or improperly maintained medical equipment can lead to adverse events.
- Patient Falls: The most frequent adverse events in hospitals, with a rate of occurrence ranging from 3 to 5 per 1000 bed-days.
- Hospital-Acquired Infections (HAIs): Affect 1 in 20 patients, often resulting from contaminated equipment or poor hygiene.
- Communication Failures: Information lost during shift changes or transfers, leading to errors in patient care.
The impact of these errors is profound. For patients, they can lead to extended hospital stays, permanent injury, or death. For healthcare providers, including physicians and other healthcare professionals, they cause immense moral distress and burnout. Financially, they cost the healthcare system billions of dollars each year.
While human error is inevitable, the systems we use to communicate can either mitigate or exacerbate these risks. Most medical errors are due to process failures and organizational factors—such as inadequate communication protocols, staffing issues, clinician burnout, and flawed institutional policies—rather than individual negligence. Addressing medical errors requires a systemic approach focused on identifying and improving flawed processes, not blaming individuals. As healthcare research and systematic reviews have shown, a study estimated that these systemic issues are major contributors to preventable harm in healthcare settings. Often, the culprit is not incompetence but “information chaos”—fragmented data that is hard to access when it matters most.

The Importance of Clear Communication in Healthcare
Communication is the nervous system of a hospital. It connects doctors, nurses, specialists, patients, and families. When this system fires correctly, care is seamless. When it misfires, patient safety is compromised. In healthcare, effective communication is essential for enhancing team collaboration, reducing medical errors, and improving patient safety outcomes. Active listening is a vital component of effective communication, helping patients feel heard and understood, which directly contributes to improved patient satisfaction.
However, healthcare communication faces significant hurdles:
- Time Constraints: Providers often have only minutes to convey complex information.
- Health Literacy Gaps: Patients may not understand medical jargon or verbal instructions.
- Cognitive Overload: Staff are often juggling critical tasks for multiple patients simultaneously.
- Written Communication: Clear, accurate, and standardized documentation is crucial for patient safety, effective hand-offs, and preventing medical errors. Proper written communication, such as legible handwriting, correct specimen labeling, and thorough discharge instructions, ensures information is accurately shared among healthcare professionals.
Clear communication also supports care coordination by unifying providers and facilitating collaboration among different healthcare teams, reducing fragmentation and enhancing patient engagement.
Visual communication addresses these challenges by making information static and persistent. Unlike a verbal conversation that disappears once spoken, visual aids remain available for reference. They bridge the gap between what is said and what is understood, providing a shared “source of truth” for everyone involved. Implementing key strategies, such as using standardized handoff communication tools like SBAR (Situation, Background, Assessment, Recommendation), ensures accurate transfer of critical information between healthcare team members. Effective communication is a key strategy to improving patient satisfaction, and achieving this requires a proactive approach that addresses communication, efficiency, and personalization.
How Visual Communication Reduces Medical Errors
Visual tools function as safety nets in the clinical workflow, supporting medical error reduction as a primary goal. By making information clear and accessible, visual communication helps prevent errors and improve patient safety throughout the care process. Here is how they specifically target and reduce error rates:
Visual communication tools, such as patient communication boards and digital displays, enhance patient care and quality by ensuring that critical information is visible and up to date for both staff and patients. These tools are supported by organizational factors—such as effective communication protocols, staffing, and safety procedures—that create an environment where visual aids can be most effective.
Patient involvement in their own care, such as verifying medication details and surgical sites, is a highly effective defense against medical errors. Visual tools empower patients to participate actively, further reducing risk.
Additionally, data visualization provides an intuitive look at patterns, trends, and outliers in health data, enabling staff to quickly identify and address potential issues before they lead to harm.
Enhancing Clarity
Medical instructions can be complicated. Visual aids simplify this complexity. A patient communication board that clearly lists “NPO” (Nothing by Mouth) prevents a dietary aide—or a well-meaning family member—from giving a patient food before surgery. When information is visual, it is less open to interpretation.
Visual aids also support personalized care by tailoring information to individual patient needs, helping to enhance patient satisfaction and engagement. Personalizing patient engagement begins with recognizing patient needs and preferences, ensuring that communication is both relevant and effective.
Minimizing Misunderstandings
Verbal orders are notorious for being misheard, especially in noisy environments. Visual cues provide confirmation. For example, a color-coded wristband indicating a “Fall Risk” alerts every staff member who enters the room, regardless of whether they have read the patient’s full chart. This reduces the reliance on memory and verbal handoffs.
Visual cues and communication boards also encourage patients to ask questions and participate in their care, which is essential for reducing medical errors. Engaged patients want to learn more about their health and have a voice in their treatment plans, making them active partners in safety and error prevention.
Improving Accessibility
In an emergency, seconds count. Searching through a digital chart on a computer terminal takes time. Visual communication ensures critical information is immediately accessible at a glance. An allergy warning displayed prominently on a whiteboard or chart ensures that a nurse administering medication sees the danger signal instantly.
In today’s digital world, digital tools such as automated prescription notifications further improve accessibility and patient safety. Automated prescription notifications help patients know when their prescriptions are ready for pick-up, when they need a refill, and how to take their medication.
Tools and Strategies for Visual Communication in Healthcare
Hospitals and other healthcare facilities are increasingly adopting a variety of visual tools to fortify their safety protocols. These tools play a vital role in supporting healthcare services by improving communication, reducing medical errors, and enhancing care coordination. Creating a comfortable environment is essential for patient satisfaction, and studies show that a clean, comfortable environment significantly impacts patient satisfaction in hospitals.
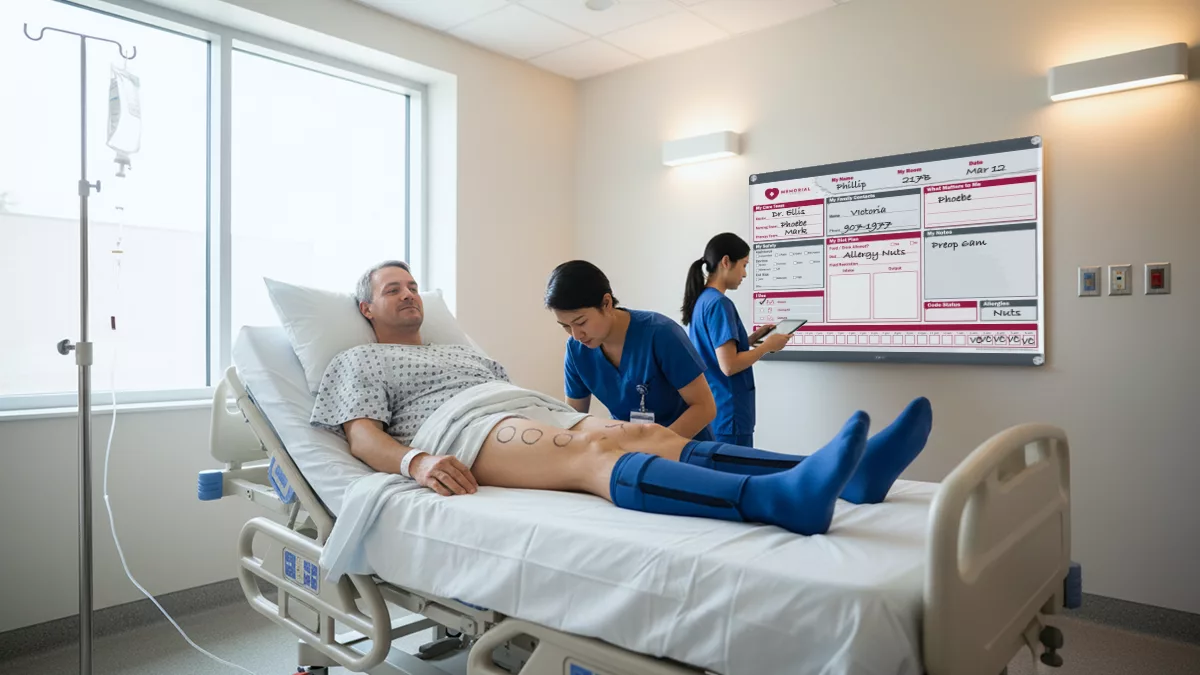
Patient Communication Boards
These are perhaps the most versatile tools in a patient room. Whiteboards or glass boards serve as a central hub for information. They typically display:
- Care Team Names: So patients know exactly who is treating them.
- Daily Goals: Keeping everyone aligned on the recovery plan.
- Pain Management Plans: ensuring consistent dosing schedules.
- Discharge Timelines: Managing expectations for leaving the hospital.
Infographics and Visual Aids
Diagrams and charts are essential for patient education. Explaining a surgical procedure using a detailed anatomical diagram is far more effective than a verbal description alone. It empowers the patient to ask informed questions, catching potential misunderstandings before they become errors.
Digital Displays and Dashboards
Digital boards outside patient rooms can display real-time isolation precautions or dietary restrictions without violating patient privacy. Centralized dashboards at nursing stations allow charge nurses to see unit-wide data, spotting bottlenecks or safety risks (like unrounded patients) instantly. By streamlining communication and automating post-discharge follow-up, these digital displays and dashboards can help lower costs and reduce operational expenses. Healthcare organizations should also explore patient satisfaction improvement plans to integrate digital solutions effectively.
Color-Coding Systems
Standardized color-coding is a simple but effective visual language.
- Red: Allergies.
- Yellow: Fall risk.
- Purple: Do Not Resuscitate (DNR).
By training staff to recognize these visual cues immediately, hospitals create an intuitive layer of safety that transcends language barriers.
Family Engagement in Care Decisions
Think of family engagement in care decisions as the heartbeat of truly patient-centered care—it’s what ensures treatment actually fits each patient’s unique values, preferences, and needs. When healthcare providers bring families into the decision-making conversation, something wonderful happens: they create this transparent, supportive environment that doesn’t just improve patient outcomes, but also boosts satisfaction and safety in ways that feel genuinely meaningful.
Here’s the thing—open communication really is everything. Healthcare organizations can absolutely foster family engagement by sharing clear, easy-to-understand information about treatment plans and genuinely encouraging questions and feedback. This collaborative approach? It’s like having a trusted guide who helps families navigate complex information, jump into care planning, and speak up about concerns that might otherwise slip through the cracks. Picture this: when families are part of discussions about medication schedules or mobility precautions, you’re actually preventing those all-too-common issues like medication errors, patient falls, and pressure ulcers.
The research backing this up is pretty compelling, too. Studies published in the Journal of Patient Safety have shown us something remarkable—when families are included in care decisions, the risk of preventable harm (think wrong-site surgery or medication errors) drops significantly. Families often become this extra layer of oversight, catching discrepancies or misunderstandings before they turn into something more serious.
Healthcare providers can tap into a variety of patient engagement tools to make this collaboration feel natural and effective. Electronic health records and patient portals—they’re like having a 24/7 window into up-to-date information, progress tracking, and direct communication with the healthcare team. Data visualization tools work their magic by transforming complex medical data into those easy-to-understand charts and graphics, empowering families to make informed decisions and dive deeper into care planning.
Leading organizations like the Joint Commission and the National Academies get it—they emphasize the need for clear communication and shared decision-making in healthcare because it works. In today’s digital world, technology opens up even more opportunities for meaningful connection. Video conferencing and mobile apps keep remote family members in the loop, while visual elements like infographics and dashboards help clarify treatment options and next steps in ways that just make sense.
Examples of Visual Communication Reducing Errors
The theory of visual safety is backed by experience. Improving internal processes, these strategies can also attract prospective patients by demonstrating a visible commitment to safety and quality care.
Reducing Medication Errors: Revamp patient rooms to include standardized dry-erase boards designed specifically for medication safety. Have the boards included a section for “Last Dose Given” and “Next Dose Due.” This simple visual cue allowed patients and families to act as a second set of eyes. In one instance, a family member could noticed a nurse preparing a dose too early based on the time written on the board, preventing a potential overdose.
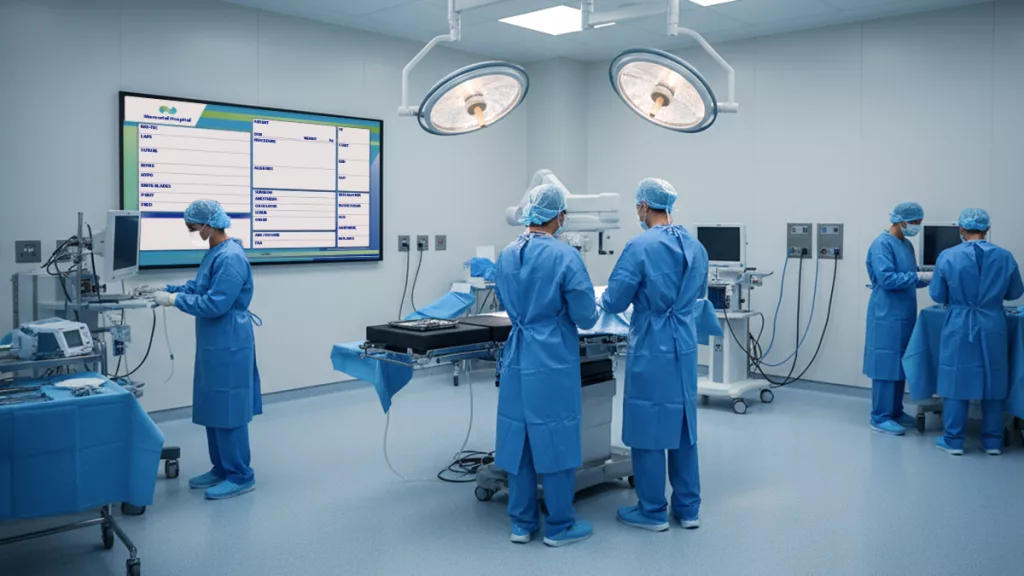
Surgical Safety Checklists: The implementation of visual surgical checklists—large custom boards in operating rooms outlining safety steps— drastically reduce surgical complications. By forcing the team to visually confirm steps like “Right Patient, Right Site, Right Procedure,” the likelihood of “never events” drops significantly.
Maintaining engagement and satisfaction after a patient leaves the healthcare facility is equally important. Patients appreciate knowing that their concerns and experiences matter, and a thoughtful follow-up can strengthen trust and foster long-term loyalty.
Best Practices for Implementing Visual Communication
To truly impact patient safety and improve clinical outcomes, visual tools must be designed and implemented correctly. Key strategies include integrating clear, standardized communication boards and digital solutions that facilitate real-time updates between staff and patients. These best practices not only help reduce medical errors but also contribute to better outcomes by enhancing healthcare quality and patient satisfaction.
In 2026, technology integration—such as AI-powered clinical decision support—will be essential for early detection of patient risks and reducing diagnostic errors. This proactive approach supports safer care environments and further improves clinical outcomes.
Designing Effective Visual Tools
- Keep it Simple: Avoid clutter. Information should be legible from a distance (e.g., from the patient’s bed or the doorway).
- Use Universal Symbols: Use icons that are easily recognized to overcome language barriers.
- High Contrast: Ensure text stands out against the background for readability.
Training Healthcare Teams
A tool is only as good as the person using it. Staff must be trained on how and when to update visual aids. Updating communication boards should be a mandatory part of bedside shift reporting, ensuring the information is always current. However, inadequate staffing can undermine the effectiveness of these visual communication tools, as overworked or insufficient staff may not have the capacity to keep boards updated, increasing the risk of medical errors and compromising patient safety.
Integrating Visuals into Workflows
Make visual checks a habit. For example, during hourly rounds, nurses should verbally reference the communication board: “I see on your board that your goal today is to walk twice. Let’s get started.” This reinforces the board’s value and ensures accuracy.
The Future of Visual Communication in Healthcare
As technology evolves, so too will our visual safety nets. We are moving toward an era of “smart” visual communication.
- Integrated Digital Boards: Future communication boards will likely sync directly with the Electronic Health Record (EHR), automatically updating vital signs, medication times, and lab results. This eliminates the risk of human error in manual transcription.
- Augmented Reality (AR): Surgeons may soon use AR overlays during procedures to visualize internal anatomy in real-time, further reducing surgical risks.
- AI-Driven Patient Education: Personalized, visual discharge instructions generated by AI could ensure patients fully understand their home care, reducing readmission errors.
Visual communication tools are increasingly being adopted in primary care settings to improve diagnostic accuracy, enhance patient engagement, and reduce medical errors. Health care systems play a critical role in supporting the adoption of advanced visual communication technologies, fostering a culture of safety and continuous improvement across all care environments. As highlighted by experts such as Meyer AN, future strategies for safer healthcare practices will rely on system-wide approaches and digital engagement to drive ongoing improvement.
These advancements promise a future where information is not just available, but proactively presented to the right person at the right time.

Clarity as a Catalyst for Patient Safety
Reducing medical errors is a complex challenge, but sometimes the most effective solutions are the most visible ones. Visual communication transforms abstract medical data into clear, actionable information.
By implementing tools like patient communication boards, clear signage, and standardized visual cues, healthcare leaders can build a safer environment. These tools protect patients from harm, shield providers from devastating mistakes, and foster a culture of transparency. Safety in healthcare begins with clarity—and clarity begins with what we can see.