Health Designer: Breaking Barriers in Modern Healthcare Innovation
Poor hospital design costs lives. A landmark study published in Health Environments Research & Design Journal found that patient-centered design improvements—better lighting, reduced noise, intuitive room layouts—can reduce medical errors more than marginal gain. That’s a fundamental shift in what healthcare environments are capable of achieving.
Health design innovation sits at the intersection of clinical expertise, human behavior, and built environments. For too long, healthcare facilities were designed around institutional efficiency—where workflows served systems, not people. That model is changing fast, and the results speak for themselves. In the broader health care landscape, health systems are under increasing pressure to adapt to new design standards that improve patient outcomes and meet evolving policy requirements.
This article is the first in a series exploring how design is reshaping every corner of the healthcare industry, from digital UX to hospital interiors to patient care environments. Across this series, we’ll examine real applications, emerging research, and the professionals driving change from the inside out, with a focus on the importance of consistency in implementing design innovations across different health systems.
By the end of this post, you’ll have a clearer picture of what health design actually is, who leads it, and how design thinking in healthcare is already transforming hospitals and care facilities across the country. Establishing best practices in health design is essential for driving operational excellence and improving outcomes in health care.
What Is Health Design—And Why Does It Matter?
Health design is a multidisciplinary approach that applies design thinking principles to solve complex challenges across healthcare environments. It spans physical spaces, digital tools, patient workflows, and care delivery systems. The goal: create environments that reduce harm, improve outcomes, and support the humans who work and heal within them.
At the center of this work is the health designer—a professional who bridges clinical needs and innovative solutions. These specialists collaborate with clinicians, administrators, engineers, and patients to translate operational requirements into functional, evidence-based design. Their ability to bridge clinical needs and deliver solutions enhances patient interactions, data management, and staff efficiency. The role demands both analytical rigor and empathy, making it fundamentally different from conventional architectural or UX practice.
Traditional healthcare planning often prioritizes compliance and cost. Health design adds a third dimension: measurable human impact. It’s iterative, informed by data, and anchored in the actual experiences of patients and staff. Health designers use insights from observational data to understand workflow patterns, interruptions, and staff responses, which inform design decisions and help track progress over time to improve reliability and safety.
The evidence supporting this approach continues to grow. The Center for Health Design’s Pebble Project—a research initiative involving hundreds of healthcare organizations—has documented consistent links between intentional clinical environment design and outcomes like shorter hospital stays, lower infection rates, and improved staff retention. One participating hospital reported a 70% reduction in patient falls after redesigning room layouts to improve visibility and access. Providing guidance to clinicians and staff during the implementation of new design solutions is crucial to ensure safety and efficiency in clinical practice.
A health designer is a specialist who uses evidence-based research to create physical spaces and digital tools that improve patient outcomes, safety, and staff efficiency.
The Role of Design Thinking in Healthcare
Design thinking is a structured problem-solving framework built on empathy, iteration, and collaboration. Those qualities make it especially effective in healthcare, where the stakes are high, stakeholder needs often conflict, and the cost of getting it wrong is significant.
The framework moves through five stages: empathize, define, ideate, prototype, and test. Applied to healthcare, this process becomes a practical engine for change. Implementing targeted strategies and procedures is essential to improve workflow efficiency and patient safety, ensuring that interventions address both operational and compliance needs.
Consider a hospital looking to reduce patient wait times in its emergency department. The empathize stage involves observing triage workflows and speaking directly with nurses and patients. Define clarifies the core bottleneck—perhaps it’s the intake form itself, or the physical location of registration desks. Ideate generates potential solutions. Prototype tests a low-cost version. Test measures results and refines accordingly. To ensure consistency and accuracy in new workflow implementations, more training for staff is often required, supporting reliable data collection and adherence to new procedures.
Healthcare workflow management is the systematic and strategic approach to analyzing, designing, implementing, and monitoring the sequence of tasks, information, and interactions that constitute healthcare processes. The primary goal of healthcare workflow management is to optimize these flows to enhance efficiency, minimize the potential for errors, reduce operational costs, and ultimately elevate the quality of patient care.
One common misconception is that design thinking is primarily about aesthetics. It’s not. When applied to healthcare, the outcomes are operational: faster discharge processes, better staff adoption of new tools, reduced readmission rates. Research published in the BMJ found that design thinking interventions in clinical settings led to measurable reductions in patient wait times and significantly higher staff satisfaction scores during implementation.
Understanding Human Factors in Health Design
When we talk about creating safer, more effective healthcare environments, understanding human factors is honestly a total game-changer. Think about it this way: human factors is all about examining how people interact with every single piece of a healthcare system—the technology, the physical spaces, the daily workflows, even the organizational culture. When we focus on these real-world interactions, healthcare design can directly tackle patient safety challenges, cut down on medical errors, and make both patients and staff genuinely happier with their experience.
You know where this becomes absolutely critical? Those high-pressure environments like emergency departments, where everything moves at breakneck speed and there’s virtually no room for mistakes. Here’s the thing—even seemingly small design oversights, like confusing signage or equipment that’s just placed in the wrong spot, can pile on extra mental stress for healthcare workers. And that cognitive overload? It leads to mistakes that could’ve been prevented. When we apply human factors principles thoughtfully, hospitals can spot these risks early and create spaces that actually support clear thinking, smooth workflows, and those life-saving quick responses.
So what does effective healthcare design rooted in human factors actually look like? It starts with really understanding just how complex patient care can be. We’re talking about designing medication systems that practically eliminate error opportunities, creating training programs that truly empower staff to succeed, and building environments where everyone—patients and clinicians alike—feels genuinely supported. Picture this: a well-designed medication room with intuitive labeling and a layout that just makes sense. That simple change can dramatically slash dosing errors and directly improve how patients recover.
Here’s what’s fascinating—implementing human factors in healthcare isn’t just about rearranging the physical space. It’s really about systems thinking at its core. This approach requires ongoing education that actually sticks, robust training that prepares people for real scenarios, and fostering a culture where open communication and continuous improvement aren’t just buzzwords—they’re daily practice. The hospitals that truly invest in human factors-based design? They often see profound changes: fewer medical errors, genuinely higher patient satisfaction, and healthcare workers who feel more resilient and supported.
Want to see this in action? The case studies really tell the story. One hospital completely redesigned its emergency department using human factors analysis, and the results were measurable—medical errors dropped significantly and patient satisfaction scores noticeably improved. Another great example: integrating user-friendly technology like digital communication boards and real-time data displays has helped clinicians juggle complex tasks more efficiently, reducing that overwhelming cognitive load while supporting truly exceptional care.
The secret to success with human factors-based healthcare design? It absolutely depends on leadership buy-in and a genuine commitment to quality and safety from top to bottom. When healthcare organizations establish clear, practical processes, provide targeted training that actually works, and foster a culture where feedback is welcomed and valued, they create environments where both patients and staff can truly thrive. At the end of the day, understanding and applying human factors isn’t just some academic exercise—it’s a practical, proven strategy for delivering quality care, improving clinical outcomes, and leading the charge in healthcare innovation.
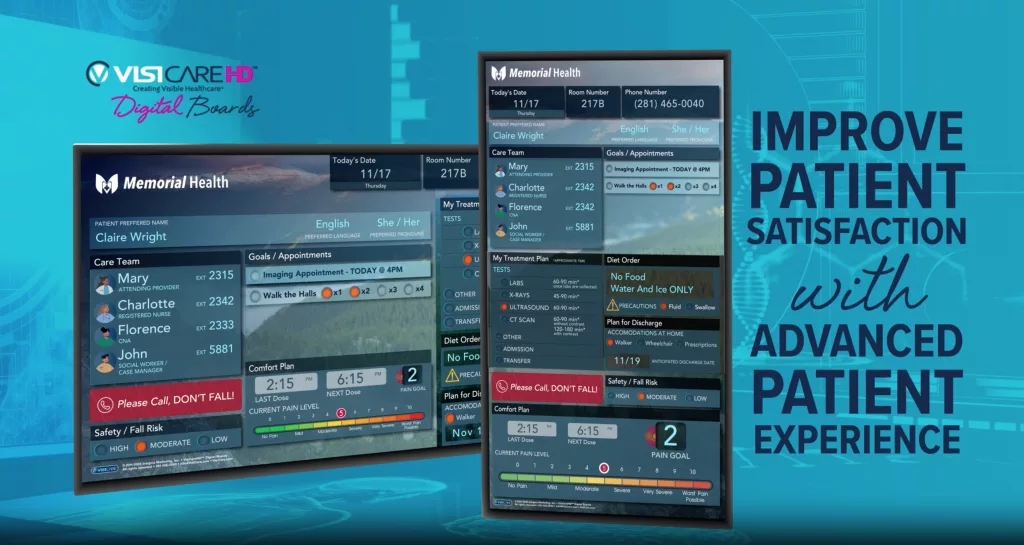
Interactive Patient Care: Where Design Meets the Bedside
Interactive Patient Care (IPC) is one of the most practical expressions of health design innovation in action. IPC systems use technology and environment to engage patients directly in their own care—turning passive recipients into active participants. IPC enhances patient experience by providing entertainment and educational resources at the bedside.
Bedside tablets, digital whiteboards, and well-designed patient portals give individuals access to their care plan, educational content, meal preferences, and direct communication with their care team. Samsung Interactive Patient Care solutions serve patients by providing access to educational content, food ordering systems, and virtual telehealth visits, streamlining patient communication and improving engagement. When these tools are designed well, the effects are tangible. Hospitals using IPC platforms consistently report higher HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems) scores and measurable reductions in call light usage—sometimes by as much as 50%.
The design considerations that make IPC systems effective are worth examining closely. Interfaces must be intuitive enough for patients who are anxious, medicated, or unfamiliar with technology. Accessibility for patients with disabilities—including visual impairments and cognitive challenges—is non-negotiable. Security features, such as those found in Samsung Knox, are essential for protecting patient data on IPC devices. And integration with existing hospital workflows must be seamless; a tool that creates new steps for nursing staff will be abandoned quickly, no matter how well-intentioned.
For Directors of Nursing and clinical managers, this last point is especially relevant. Well-designed IPC tools reduce the administrative burden on care teams, freeing nurses to focus on direct patient care rather than fielding routine requests. IPC solutions can integrate with EMR and hospital IT systems, leveraging administrative data to improve patient-centric applications and service delivery. That’s not a secondary benefit—it’s a direct response to one of the most pressing pain points in clinical management today.
Community-based approaches in IPC foster interdisciplinary collaboration among healthcare teams, improving workflow efficiency and enhancing patient safety through shared knowledge and coordinated efforts. The efficient use of resources—including staff time, equipment, and data—during IPC implementation is critical to maximizing financial health and care quality. Training and engagement of healthcare staff are essential for the successful adoption of IPC and communication products. Continuous monitoring and feedback help optimize the use of IPC and communication systems. Patient communication systems can also provide access to language and interpretation services, improving communication clarity for diverse patient populations. The growth of the IPC market is driven by increasing demand from the elderly population and newly insured individuals. IPC solutions help hospitals meet service and quality requirements, while improving patient satisfaction and outcomes through better education and empowerment.
Collaborative Medical Design: Breaking Boundaries Through Partnership
The most impactful health design innovations don’t come from a single discipline. They emerge from genuine cross-disciplinary collaboration—bringing together clinicians, administrators, designers, engineers, compliance officers, and patients in the same room, working toward the same goal.
Effective collaborative medical design looks like co-design workshops where frontline staff prototype new workflows before implementation. It looks like patient advisory councils providing input on room configurations. It looks like rapid iteration cycles where a new nursing station layout is tested in a mock-up environment before construction begins.
Involving frontline staff early is not just good practice—it’s the difference between adoption and resistance. Nurses, technicians, and administrators bring irreplaceable knowledge about day-to-day operations. Involving physicians in the design process is also critical, as it helps address workflow challenges and reduces the impact of multitasking and interruptions on physicians’ error rates and overall care quality. Solutions designed without their input often fail at the implementation stage, creating costly rework and eroding trust in future initiatives.
Healthcare design consulting firms increasingly operate as embedded partners within hospital systems, co-developing solutions rather than delivering finished products. This model reduces implementation risk significantly. When a design team has worked alongside clinical staff for months, the resulting solution reflects operational reality—not just a best-case scenario.
Compliance is another area where early collaboration pays dividends. Design processes that involve compliance officers from the outset are far more likely to produce HIPAA-aligned solutions without expensive revisions. Regulatory alignment, built in rather than bolted on, is one of the clearest indicators of a mature, patient-centered design process.
Healthcare Design in Action: Real-World Applications
Theory only goes so far. Here’s how health design innovation is making a tangible difference in hospital settings right now. Tracking progress over time is essential to assess the effectiveness of these health design interventions, ensuring that improvements are measurable and sustained.
Wayfinding and Spatial Design: Patients who can’t navigate a hospital experience higher anxiety levels and are more likely to miss appointments. Intuitive wayfinding—clear signage, logical spatial flow, distinct visual zones—reduces patient stress and improves operational efficiency by decreasing the volume of directional inquiries staff must handle. Simple design decisions, like color-coded corridors or strategically placed maps, have measurable downstream effects on patient experience and facility throughput.
Digital Workflow Tools: User interface design directly influences whether clinical staff adopt new systems or work around them. Tools with cluttered layouts, unclear labeling, or poor mobile optimization create friction that leads to errors and workarounds. Hospitals that invest in usability testing and iterative UX design for their digital tools see higher adoption rates, fewer input errors, and faster onboarding for new staff.
Environment of Care: Material selection, room configuration, and acoustic design all affect patient recovery times and infection control outcomes. Private rooms with natural light, surfaces that support effective cleaning protocols, and layouts that minimize cross-contamination are not aesthetic choices—they’re clinical ones. A future article in this series will explore Environment of Care design in depth, including how these decisions interact with infection prevention strategy and staff wellbeing.
Each of these applications directly addresses the priorities hospital administrators and clinical managers measure: improved patient outcomes, enhanced staff collaboration, and reduced operational costs.
Frequently Asked Questions
What does a health designer do?
A health designer applies design thinking to healthcare challenges—working across physical environments, digital systems, and care workflows. They collaborate with clinical and administrative stakeholders to develop solutions that are human-centered, evidence-based, and operationally sound.
How is design thinking used in hospitals?
Design thinking is used to redesign patient intake processes, optimize ICU layouts, improve digital tool usability, and develop staff-facing workflows. Its five-stage framework—empathize, define, ideate, prototype, test—provides a structured method for tackling complex, high-stakes problems in clinical settings.
What is the ROI of health design innovation?
Documented benefits include reduced patient falls, shorter hospital stays, lower infection rates, higher HCAHPS scores, and improved staff retention. The financial returns vary by intervention, but the Center for Health Design’s Pebble Project has consistently linked design investment to measurable clinical and operational improvements.
What is Interactive Patient Care?
IPC refers to systems and tools—such as bedside tablets, patient portals, and digital whiteboards—that engage patients directly in their own care. Effective IPC design improves communication, reduces call light usage, and increases treatment adherence.

The Future of Health Design Starts Now
Health design innovation has moved well past the “nice to have” stage. The evidence is clear: patient-centered design drives better clinical outcomes, stronger operational performance, and measurable financial returns. Design thinking, collaborative medical design, and interactive patient care are not isolated initiatives—they are interconnected pillars of a healthcare environment built around the people it serves.
For healthcare administrators and clinical managers looking to act, three practical starting points stand out. First, conduct a design audit of your current patient care environment—identify where physical or digital friction is creating avoidable stress for patients and staff. Second, select one workflow or space where a design thinking approach could deliver near-term improvements. Third, bring frontline staff into co-design conversations early. Their operational knowledge is an asset no consultant can replicate.
The healthcare facilities that will lead in the next decade are already rethinking how design shapes care. The question is not whether health design innovation matters—the evidence has settled that. The question is how quickly your organization is prepared to act on it.
Comments (4)
Comments are closed.



Where Health Meets Space in Wellness Design | VisiCare
April 16, 2026[…] Effective wellbeing design doesn’t happen in silos. It requires multiple disciplines working in coordination, each contributing a distinct lens to the overall environment. Designers—including architects and interior designers—play a crucial role in shaping wellness-oriented spaces, and collaborative design processes are essential for achieving holistic outcomes. Technologies such as generative AI tools and interactive systems are transforming wellness design by streamlining workflows, enabling greater personalization, and fostering innovation. […]
10 Healthcare UX Design Trends Transforming 2026 | VisiCare
April 23, 2026[…] of health design and human factors as your trusted foundation for creating healthcare UX that actually works in the real world—the […]
The Nurse's Guide to Healthcare Design: Your Voice Matters | VisiCare
April 30, 2026[…] to align design solutions with their needs and expectations, ensuring that every aspect of the healthcare environment design supports comfort, safety, and the overall healing […]
Master Interactive Patient Care for Better Safety | VisiCare
May 7, 2026[…] insight into the role of innovative design in supporting safe, effective care settings, explore Health Designer: Breaking Barriers in Modern Healthcare Innovation. By prioritizing a safe care environment, healthcare organizations can reduce risks, improve […]